Project Leader: Greg Smith
Repeated exposures to ozone have been shown to cause eosinophilic airway inflammation in multiple species. These findings provide one potential explanation for how ozone could cause asthma. Utilizing an ozone exposure paradigm developed by our collaborator Jack Harkema at Michigan State University that produces phenotypes of non-atopic asthma, we screened strains from the Collaborative Cross to test whether genetic variation influences this response. Indeed, we found marked variation across strains, indicative of gene-environment interaction. One CC strain, CC002, exhibited by far the strongest response to ozone (see Figure), and we are now hunting down the genes that render this strain susceptible. By identifying these genes and the pathways they participate in, we will gain crucial insights into how ozone can cause asthma.
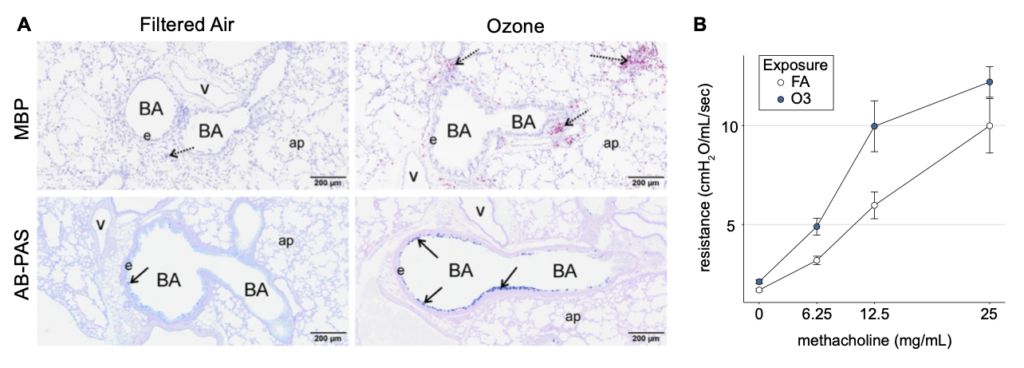
(A) Representative histological sections of filtered air (FA) controls and ozone exposed CC002 mice showing (top) peri-bronchial eosinophilic inflammation, detected by IHC for major basic protein (MBP, red stain), and (bottom) mucous cell metaplasia in bronchiolar epithelium as detected by Alcian blue-periodic acid–Schiff (AB-PAS) staining. Histology key – BA: bronchial airway, e: epithelium, ap: alveolar parenchyma, v: blood vessel. Arrows denote regions of airways featuring eosinophils or mucous cells. (B) Elevated lung resistance at baseline and after escalating doses of methacholine in ozone exposed (vs. FA control) CC002 mice, indicative of airway obstruction and hyper-responsiveness, respectively, which are hallmark phenotypes of asthma.